Victory Friday | Issue 125
Orthopedic Insights: (Unrecognized) Chronic Pain Risk Factors • Conor’s Cross-Legged Hip Opener • Hip-Hinged Run Stride Coaching • “Energy In, Energy Out” With the Elbow
“Small deeds done are better than great deeds planned.” ~Peter Marshall
Victory Friday is a weekly digest of reflections, insights, and tools from the world of functional manual and performance medicine. It is a free weekly publication. To support Victory Friday with a paid subscription, click below:
Trauma is the theme of this week’s Victory Friday! Nothing dramatic, but therein lies the problem: often we have moderate (or even mild) falls that can cause longstanding problems: stubborn elbow pain in skateboarding kids, or lost joints in the elderly. Thus, the concept of “Energy In, Energy Out” is so crucial. Read on to find out more!
What I’m Into: (Unrecognized) Chronic Pain Risk Factors. The common belief in Western medicine that chronic pain — often leading to surgery or joint replacement — is just “a normal part of life” or an inevitable consequence of “being very active” is a bogus one.
Chronic pain usually arises from a combination of factors. One major but frequently ignored contributor is old, seemingly healed injuries.
These past injuries often lead to subtle, compensatory movement patterns that create ongoing strain, eventually causing persistent pain and, in many cases, the need for major surgery.
How do I know this?
When I ask clients to tell me, “When did your knee pain begin?”
its originals can often be traced back to a past trauma.
Here’s a list of common (but often overlooked) past injuries—and the chronic pain conditions or major surgeries they frequently contribute to later in life:
Bad Ankle Sprains & Falls on a Hip:
• knee pain and total knee replacement
• hip pain and total hip replacement
• chronic low back pain and lumbar surgery
Why: full and efficient ankle mobility is critical to the efficiency of the whole leg. Ankle sprains often alter the joint alignment and motion of the ankle, with chronic repercussions that transmit up the leg.
• Bad ankle sprains: Inversion sprains are common but “heal” fairly quickly, usually requiring brief periods of rest followed by gradual resumption of activity.
But the biggest chronic outcome of a bad ankle sprain is lost dorsiflexion: when the tibia and fibula fail to glide efficiently over the talus bone.
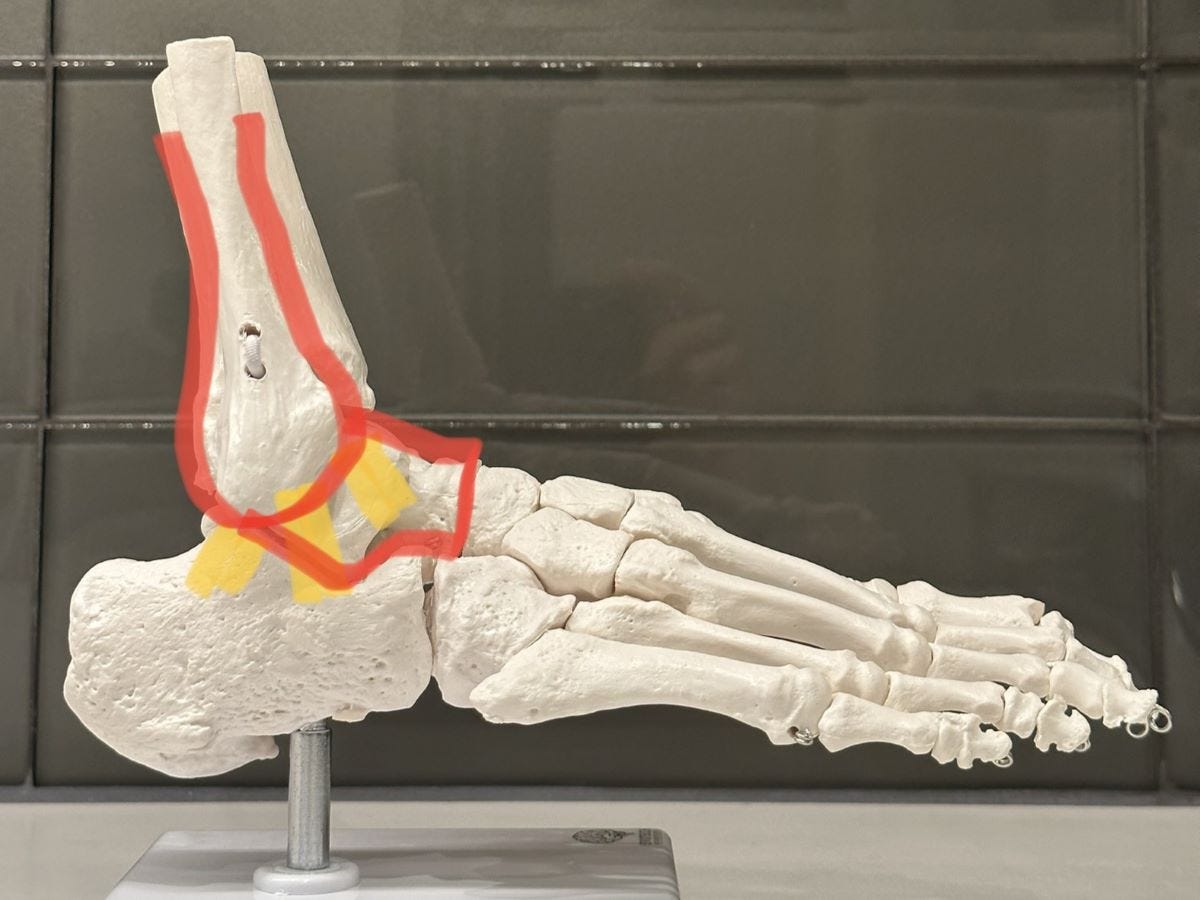
A loss of efficient dorsiflexion may cause excess tibial rotation (stressing the knee with torsion and shear forces).
Torsion and/or shear between the tibia and femur causes relentless strain that — over a long enough period — may cause chronic pain, degenerative changes to the cartilage and menisci of the knee, and often result in surgery.
Chronic ankle dorsiflexion loss automatically limits hip extension: the foot needs to stay on the ground (and ankle bend) in order to access the full push-off in walking and running.
Even subtle ankle stiffness can reduce hip motion, resulting in hip and low back strain.
And again, chronic dorsiflexion mobility loss may result in chronic strain, leading to chronic pain, degeneration and potential surgeries.
Falls on the hip. Falling on the hip or pelvis — the side or the back — is super-common occurrence. While these falls may cause serious fractures in the elderly, even medium-hard falls among younger people may result in only minor pain but significant biomechanical changes.
A hard impact on the hip may result in one or more of the following:
• compression and mobility loss at the hip (femoral-acetabular) joint
• compression, malalignment and efficiency loss at the pelvis (sacroiliac joint)
Like with the ankle, the “ouch” (local inflammation and pain) usually dissipates quickly; but efficient alignment and motion seldom corrects automatically.
Once this “wheel” stops moving sufficiently (or efficiently), pain can result at the hip, above (lumbar) and below (the knee).
Head, Neck, Ribcage Impacts. Severe head and neck trauma, like concussions and whiplash, are serious injuries that often result in severe pain and disability, resulting in long recoveries.
But many mild- to moderate traumas to the head, neck and ribs are easy to shake off, but can create longstanding issues, including:
• neck and extremity radicular pain (and cervical surgery)
• shoulder pain (and shoulder surgery or replacement)
• low back and hip pain (and surgeries)
Why: impacts to the head and neck can create local problems, but the structural and fascial relationships are what often cause longstanding problems, both regionally and more globally.
• Head and neck traumas can result in chronic mobility loss in the joints and soft tissue of the neck, causing chronic neck pain.
But craniocervical trauma can also cause sneaky-but-profound problems in the shoulders, upper back and even lower body, through the cervical fascial system1. This often includes the most stubborn and seemingly intractable low back and hip pain.
• ribcage traumas often smart, result in a few days (or weeks) of impaired movement and breathing, then “heal”. Yet frequently this system — and various tissue layers — fails to align and move properly, causing all sorts of problems.
A stiff, post-traumatic ribcage is a huge issue in chronic shoulder pain: ribs need to move, and if they get stuck in elevation or posteriorly, they often block efficient scapular positioning and movement—a major factor in shoulder pain that is commonly overlooked2.
But because of the multiple key fascial systems — both external (thoracodorsal fascia) and internal (endothoracic fascia) — ribcage traumas can cause longstanding and severe issues, particularly in the lumbar spine, pelvis, hips — and by extension — the knee and the rest of the leg!
A stiff, dysfunctional ribcage often creates tension in these fascial layers, causing range of motion loss at the pelvis it connects, too, and compressive forces at the lower spine.
Old, unresolved ribcage injuries play a huge role in chronic low back, hip and knee pain.
Takeaways:
• Traumas are Trouble! High-energy stresses — such as falls — cause tissue strain: bruising, tearing, breaking. These typically heal with rest3…but that high-energy impact nearly always causes altered bony alignment and joint motion.
These post-traumatic inefficiencies, more often than not, persist indefinitely unless a significant, focused mobilization restores it: “Energy In, Energy Out.”4
• Look for system dysfunctions in problem areas: look above and below for shoulder, lumbar, hip and knee pain. Care about the whole system and you’re more likely to find subtle (and often asymptomatic) dysfunctions in yourself and your clients.
• Ask about - and dismiss at your own peril - old trauma histories! All old traumas matter until that injured area is evaluated!
Cool Exercises I Like. Conor’s Cross-Legged Hip Opener. The best way to improve joint mobility is to expand its joint space. This increases space allows the bone — in the case of the hip, the “ball” of the femoral head — to move in every direction, farther, easier and with less pain.
And since the early days of Victory Friday, I’ve advocated for strategies that stretch open the back of the hip joint — what I call “the Posterior-Inferior-Lateral Corner” (PILC5).
It’s so crucial for the hip: not just for motion, but also maximum glute strength and athleticism.
Yet, we abuse that area by…sitting on it all day!
As such, I’m constantly looking for different strategies to effectively open that area.
This recent share from trainer and biomechanist Conor Harris (@conor_harris_) highlights one of my favorites: a cross-legged, kneeling hip stretch:
This technique uses gravity and the ground to drive the femur into that posterior-inferior-lateral space, to stretch it open. This space-generating strategy opens up all motions of the hip, and puts the glute muscles in an optimal position for peak strength.
Never stop stretching and strengthening into The PILC!
Joe’s Articles. Hip-Hinged Run Stride Coaching. The high school track season began this week.
Optimizing running form is central to the skill development arm of my coaching philosophy. And there are two parts of running form:
Posture: how the body is positioned and aligned in space.
Propulsion: how the arms and legs move, on the body and on the ground.
Of the two, posture is more important:
The position and alignment of the spine and pelvis will largely dictate what the arms and legs do. So that is always the starting point.
Every athlete I coach — and treat in the clinic — gets educated on hip hinge: the concept of positioning the pelvis slightly behind the rest of the body:


A few Victories back I shared my first piece on hip hinge running posture. In response to comments and debate, I released a follow-up on iRunFar.com:
Hip Hinge, Part 2: Balance, Integration, Propulsion, and Strengthening
TL;DR: The key points from that article, and for you to consider when optimizing for hip hinge, versus other posture and positional strategies.
Hip Hinge vs. ‘Running Tall’
“Running tall” often means neutral straight posture (ear-to-hip alignment) to avoid slumping, but extreme upright/vertical trunk with lumbar extension can cause issues.
Problems with overly “tall” posture include trunk extensor dominance, reduced anterior core activation, loss of hip hinge, over-striding, and higher landing forces.
You can maintain a “tall” neutral spine while still using a forward-oriented hip hinge.
Hip Hinge vs. Pelvic Tilt
Hip hinge is isolated at the hip joint—no pelvic motion needed.
Pelvis should stay relatively perpendicular to the spine; extreme anterior or posterior tilt isn’t required for effective hip hinging.
Food for thought when optimizing yours — or your athletes’ — running form!
Victory Friday. “Energy In, Energy Out” With the Elbow. Whenever I address a new pain or injury, I always:
• ask about any relevant trauma history
• get the full story, including the most precise description of the mechanism: how the body was impacted, what direction the body or force was directed
This can tell you a lot about how to relieve pain and restore function: using hands-on techniques or exercise to reverse the traumatic “Energy In”6.
And in the case of elbows, it may tell you everything you need.
Elbows are fun to treat: true elbow — humeral-ulnar — joint pain is rare; and assessment and correction of the joint alignment can result in rapid improvement of even the most stubborn pain and mobility loss.
Most humeroulnar joint pains occur after trauma. Consistent with the chronic pain theme above, high-energy falls both cause acute tissue irritation or damage, but also input enough energy to compress, mal-align or otherwise change the alignment and movement efficiency of the joint.
When instructing on elbow treatment, my mentor and Institute of Physical Art Founder Gregg Johnson taught us that:
The key to treating a post-traumatic elbow is mobilize the ulna in
the reverse direction of the traumatic impact.
Most falls are forward “falls on out-stretched hand” (FOOSH). As such, the hand or forearm strikes the ground, first, driving an upward, compressive force into the humeroulnar joint.
Thus the most important mobilizing force for a FOOSH mechanism is traction: distracting the ulna (olecranon) away from the humerus (olecranon fossa):
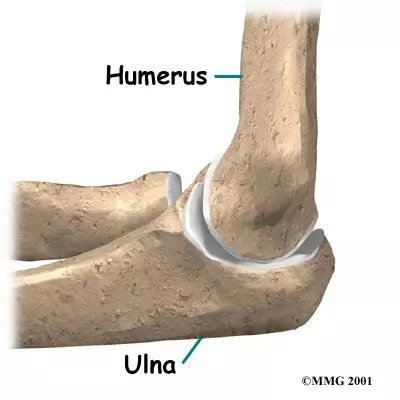
But what if their fall wasn’t a true FOOSH?
The Skateboarders Elbow. Several years ago on Fellowship I treated a middle school boy for elbow pain. He noted that it began after falling on it.
“How’d you fall on it?”, I asked.
“Skateboarding”, he said.
The elbow lacked full flexion. Palpation of the olecranon process found that the olecranon failed to “fully bury” into the fossa — another key strategic efficiency metric from Gregg.
For the first visit, I focused on various joint mobilizations that emphasized traction. Mobility improved modestly and he felt a little better. I prescribed both elbow flexion exercise and some traction: bar-hanging.
But when he returned for the second visit, he noted his elbow didn’t feel much better. Nor was it moving better, despite the treatment and home exercise.
I was missing something. I went for more clarification.
“When you fell skateboarding, how did you fall?”
“Oh, I went off a jump, landed, but fell backwards.”
He then demonstrated, indicating that he hit directly on the “elbow point” (olecranon process) — in such a way that, the ulna would have translated inferiorly, or driven away from the humerus!
The opposite of how I was treating it.
🤦🏻♂️

Thus, I reversed course. I performed flexion mobilization with an emphasis on compression: gliding the humorous superiorly, “into” the elbow joint.
By visit’s end, his flexion motion was fully restored, he had no pain with movement, we were both happy, and I never saw him again.
Take-Aways. Mechanism is Everything, Especially in Elbows! The true needs of a joint — particularly the small joints of the hand, wrist, forearm and elbow — can sometimes be difficult to assess.
And it’s easy to assume fall trauma is compressive! Yet this is a rare case where the traumatic force created a distraction strain. And thus, a compressive mobilization was key to a rapid and full recovery.
Issue 125 is a wrap!
Help people move, function and feel better: please share this publication!
Thanks for reading, and have a great weekend,
Issue 26: Joe’s Cranio-Cervical Treatment Strategy. My multi-dimensional treatment strategy for the craniocervical, orthopedic and neuro-fascial system: treat the layers (scalp, bones and sutures, subcranial fascia and tissue), correct the cranial torsion, then restore efficiency to the cervical spine.
Issue 31: Advanced Cranio-Cervical Care. A video demo (and potential how-to) treat the cranium.
Issue 23: The Shoulder Landscape. The “Shoulder Landscape” analogy advocates treating persistent shoulder pain from the core outward: first restore smooth mobility and positioning in the thoracic spine and ribcage (“the foundation”), then improve shoulder blade stability (“the crane base”), cervical integrity (“power supply”), and finally work directly on the shoulder joint itself (“the crane arm”). Sustained pain relief and optimized efficiency of the shoulder requires this systems-based approach.
or surgery plus rest.
A maxim from my friend and colleague Garrett Petry, describing how high-energy traumatic injuries often require aggressive (high-energy) tissue mobilization to fully correct.
Issue 2: The PILC. The posterior-inferior-lateral aspect of the hip joint capsule is the area of the joint — the “back-bottom-outside corner” — that needs to be accessed to put the glute musculature at ideal stretch, while helps activate the group for optimal use.
See #4.