Victory Friday | Issue 128
Orthopedic Insights: “Low Effort, Low Pain, High Yield”: Gold Standards for Mobility Exercise • Anti-Aging Strength Work • “Hammer Don’t Hurt ‘Em”: Thoracic Mallet Manip Frees a Stubborn C-Spine
“You create what you think, so choose to think about what you wish to live.” ~ Paching Hoé Lambaiho
Victory Friday is a weekly digest of reflections, insights, and tools from the world of functional manual and performance medicine. It is a free weekly publication. To support Victory Friday with a paid subscription, click below:
The theme of this week’s Victory Friday: successful side door strategies for full and pain-free mobility! Mobility is crucial for function, and motion loss is frequently painful. But restoring motion needn’t be torturous. In fact, doing the right thing is often painless, easy, and highly effective. But those doors are hidden. I’ve mapped a few, below — check it out.
What I’m Into: “Low Effort, Low Pain, High Yield”: Gold Standards for Mobility Exercise. When prescribing home exercise to clients or athletes, I am highly empathetic. I consider:
• Would I (or do I) do this, myself?
and
• Will it deliver immediate, measurable results? (Is it coffee or vitamins?1)
But mobility…hurts. And it can take a lot of effort.
But worst of all? For many of us (yes, including me), most mobility work is ineffective. You don’t actually move any better. Or hardly at all.
I couldn’t tell you how many sun salutations I have done in yoga, yet my toe-touch mobility never improves…with toe-touching.
That goes for any hamstring stretch. Whether it’s standing, long-sitting, or lying down (with a belt), stitching hamstrings seems to yield hardly any improvements.
Is there anything worse than a stretch that:
• is super-painful
• takes a lot of effort, AND
• results in negligible improvement?
Yet a lot of physios and others in the performance and rehab spheres are dead-set on prescribing such futile options.
But not me. Not any more.
I no longer prescribe mobility work unless it is:
• low-effort
• low pain
• high-yield
That’s a high bar to clear. But achieving these mobility gold standards is easier that many realize. Here’s how:
Fascia, First. Most mobility exercises fail because they attempt to stretch fascia that is too dense, too cold, and too dehydrated. So in order to have any shot at improving mobility, we must first mobilize the fascia: heat, soften and hydrate.
This typically involves tissue mobilization using tools: foam roll, balls, hands-on techniques. Getting onto and into the fascia and applying friction energy.Access the Side Doors. Doing “the motion” to improve “the motion” might seem logical. But so might pulling on ends of a shoelace knot. Even the most essential motions — hamstring elongation, shoulder flexion — require multidmineisnoal strategies to unlock the movement of interest.
In other words, in order to access the front door, we need to enter through a side door, first.
Besides the toe-touch, one of the most painful, difficult and nausea-inducing exercises to “improve” shoulder flexion is the door pulley exercise:

This exercise is a common prescription for a stiff post-surgical shoulder, or for the diagnosis of frozen shoulder: both conditions that often result in severe (and stubborn) overhead flexion mobility loss.
The pulley exercise is (passively-and-aggressively) “doing the motion to improve the motion”: a front door strategy that is often incredibly painful.
Why? Because flexion mobility loss is often a result of lost glenohumeral arthrokinematics: the subtle-but-crucial adjustments the humeral head (“ball”) must do to stay centered in the socket as the humerus moves. For flexion, the ball of the shoulder loses the ability to “spin” (“roll and slide”) as the humerus elevates:
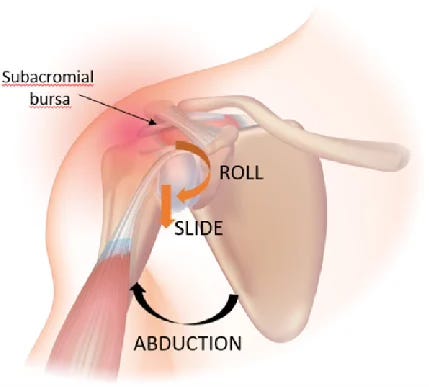
So what does a pulley do?
The pulley jams the humeral head even more into the acromion!
This is why it tends to create a lot of pain (for a lot of effort) and not amount to much mobility improvement.
This is akin to a “jammed” (if not “locked”) front door. You can choose to bash into it in hopes that it’ll budge open, but, again, it’ll require: high effort, high pain and low (or at least slow) yield.
Among my favorite side doors for shoulder elevation is this exercise:

This mobilization — using a high-resistance monster band — applies a lateral traction force on the humeral head. This decompresses the joint and gives the ball more room to “spin” in the socket, improving flexion — with less effort, less pain and more sustained gains.
Here are some other common examples of difficult, painful and low-yield stretches, and my low-effort, low-pain and high-yield alternatives:
Hamstring:
• Tired: seated toe touch; supine belt pulls
• Inspired: lateral quad massage and stretching (liberating the nearby hamstring from tight quads2); tennis or lacrosse ball massage to quadratus lumborum
Hip extension (“tight psoas”)
• Tired: lunge or couch stretching
• Inspired: visceral mobilization (belly ball) and my quad/hip stretch
Ankle dorsiflexion
• Tired: wall calf stretch
• Inspired: belt ankle mobilization
I recently restarted a weekly mobility class at my physio office. For the one hour of class, about 45 minutes of it is fascial mobilization and various “side door” strategies.
It is very popular because it is: low-effort, low-pain and high-yield! Just as mobility work should be.
Once you understand and fully appreciate the profound interconnectedness of the fascial system — and the far-reaching changes you can achieve — you begin to realize how many powerful “side doors” exist in the body:
• toe, foot and shin fascia to improve hip and lumbar flexion
• lateral ribcage foam rolling to restore shoulder and hip motion
• medial and lateral hip myofascial release to improve hip flexion and extension
Doors that hold the key to unlocking crucial — and heretofore hopelessly stubborn — mobility restrictions.
Cool Exercises I Like / Joe’s Articles. The Fountain of Youth, Part I: Strengthening 4 Anti-Aging Muscle Groups. A benefit of being a Substack author and reader is the platform’s recommended readings.
This gem fell into my lap this week, from @Varianavolk:
4 Muscles to Train for Maximum Anti-Aging Effect
Graceful aging is a major professional (and personal) priority. And this post outlines four of the most crucial muscle groups to train in order to promote high-level function, and prevent significant decline and age-related challenges, as you age.
TL;DR:
Targeting the gluteus maximus, spinal extensors, soleus, and tibialis anterior delivers maximum anti-aging benefits by preserving metabolic efficiency, posture, circulation, gait stability, and independence as sarcopenia accelerates after age 30.
The Four Key Muscle Groups:
Gluteus Maximus:
• what it is & why it’s important: largest muscle in the body and one of the biggest glucose disposal sites; critical for pelvic stability, hip extension, preventing lower-back pain and postural collapse, and maintaining healthy blood-sugar regulation to avoid insulin resistance and metabolic slowdown.
• how to train: walking lunges, Bulgarian split squats, barbell hip thrusts, squats, and back extensions on a 45-degree bench.Spinal Extensors:
• what it is & why it’s important: deep muscles (erectors, multifidus) that hold the spine upright, protect vertebral discs through loading/unloading cycles, maintain lung capacity, support oxygen/CO₂ exchange, and prevent forward collapse that impairs breathing and oxidative metabolism.
• how to train: back extensions on a Roman chair, prone extensions from the floor, deadlifts (especially Romanian), unsupported rows, bird dogs, and Pallof presses.Soleus:
• what it is & why it’s important: deep slow-twitch calf muscle that excels at continuous oxidative glucose burning for superior blood-sugar control and acts as a “peripheral heart” to pump venous blood upward, improving circulation and reducing cardiac workload.
• how to train: seated calf raises, soleus pushups, wall sits, and heel raises at the bottom of squats.Tibialis Anterior: shin muscle responsible for ankle dorsiflexion; essential for proper gait, toe clearance during walking, impact absorption at heel strike, and fall prevention—the leading cause of injury-related death over age 65.
• how to train: tib raises (wall or seated with weight), walking on heels, and tib bar loaded dorsiflexion.
Prioritizing these four muscle groups (with as little as 20 minutes, three to four times per week builds the foundational resilience that keeps you metabolically healthy, mobile, and high-functioning!
Victory Friday. “Hammer Don’t Hurt ‘Em”: Thoracic Mallet Manipulation Frees a Stubborn Cervical Spine.
One of my colleagues, a brilliant, innovative nerve and vascular manual therapist likes to say:
Today’s magic is tomorrow’s science.
Such a statement makes me feel at ease when I utilize certain treatment strategies, achieve profound results…yet I cannot explain with any certainty why it worked.
A great example of this occurred this week.
A client and old friend checked in this week, a month since his last visit, and fresh off a three-week rafting trip. He has a complex spinal pain history that includes two major lumbar surgeries, but also innumerable moderate to severe head and neck traumas.
He notes that, near the end of the trip, the oar of the raft he was paddling got caught in some underwater debris, resulting in a traction strain — through his outstretched arm, and into his neck and upper back. His pain was significant for several days and was still lingering when he showed up.
Cervical mobility testing showed:
• 35 degrees of sidebend right
• 25 degrees of sidebend left (with compensatory hiking of the upper ribcage)
• 60 degrees of left rotation
• 45 degrees of right rotation
To palpation, there was profound — and very painful — tension in the scalene and cervical paraspinal muscles, bilaterally (but right significantly more than left).
And passive motion testing — sidebending and rotation — in supine was no better. His neck was indeed locked-up!
Assessing joint motion: there was substantial mobility loss in both uncovertebral (medial/lateral shear; side bending) and facet (extension) motion — also bilaterally, but also right much worse than left.
The stiffness was suggestive of an acute-on-chronic strain: higher tissue tone around pre-existing — and seemingly longstanding (and stubborn) — joint mobility deficits.
I began treatment by addressing the myofascial tension in the neck. The right side was almost too painful to treat, so I worked to free stiff tissue on the left side: hoping this liberation would free the opposite side. It was marginally helpful.
I worked the right side, but both pain and tone remained high.
So, based on the teaching and mentorship of Institute of Physical Art Founder Gregg Johnson I addressed mobility restrictions in the upper thoracic region. In the IPA paradigm, the upper thoracic is a foundational structure that often perpetuates — if not creates — cervical dysfunction. As such, “clearing” the upper thoracic spine of dysfunction is a key aspect of neck treatment.
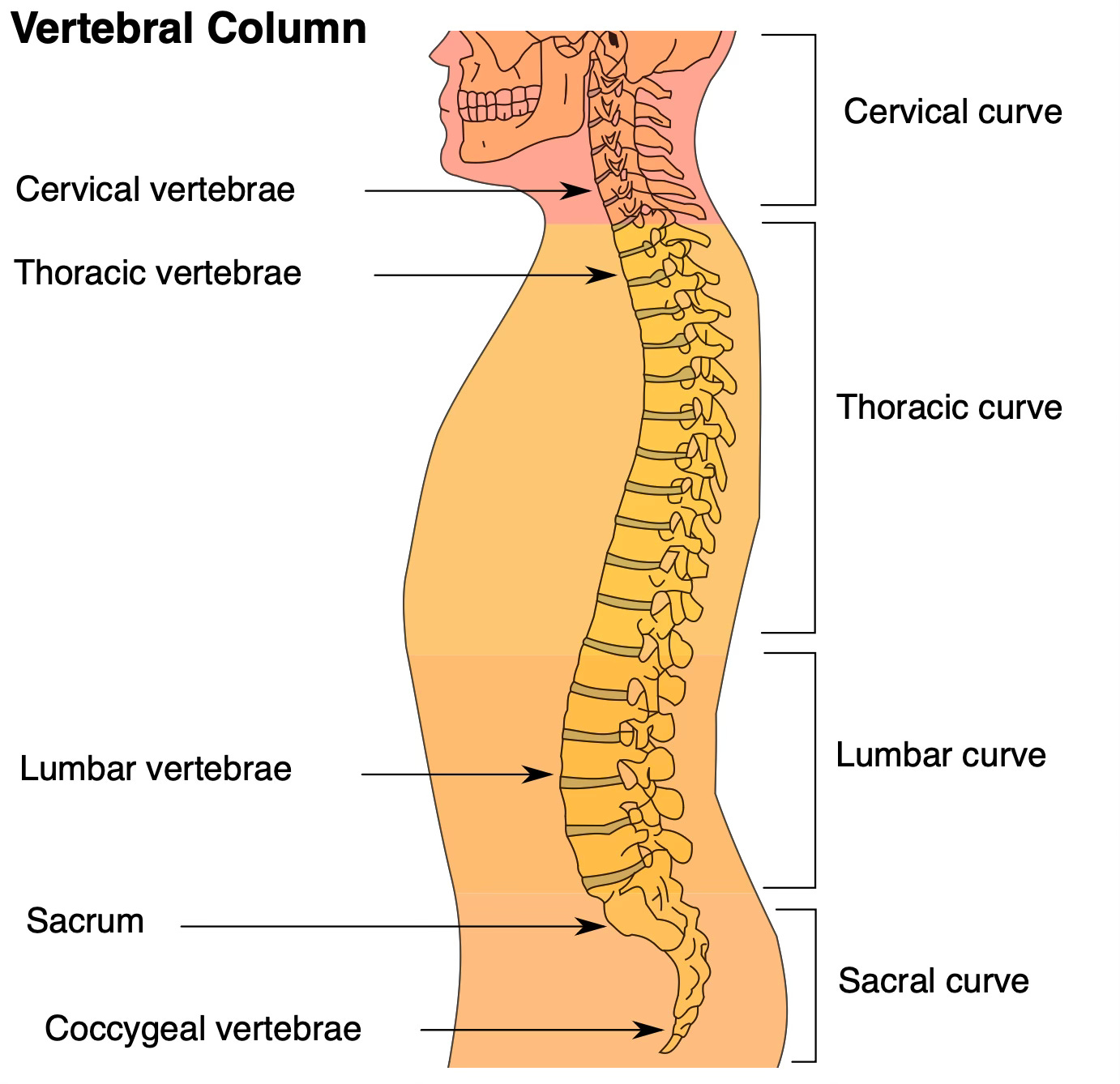
Typical of active, 40+ year olds, his upper thoracic spine was restricted: lacking in multi-directional motion including extension and rotation (and lateral shear, a key component of rotation).
And since this upper thoracic restriction was neither sensitive or a primary part of the strain injury, I chose to treat it aggressively: using my rubber mallet and rubber-tipped chisel.
I refer to this technique as “mallet manipulation.” Using a mallet and chisel, I apply a high-velocity, low-amplitude force (high speed with a very small movement) directly to the vertebral joint. This produces a quick “pop” or “crunch” similar to a common chiropractic manipulation.
Because of the chisel’s small size and the ability to position and aim it with high precision, mallet/chisel manipulation can be significantly more effective and carries less risk of collateral effects compared to a broader, high-amplitude “big pop” adjustment.
In some ways, the head of the chisel resembles the tip of today’s popular massage guns. However, unlike massage guns—which deliver repeated, rapid impacts—the mallet technique is far more conservative and targeted, even though it may appear unconventional or even intimidating.
Lastly: anyone skeptical about the role of thoracic manipulation for neck health, the medical evidence is stout: it is hugely impactful.
So I got to work.
In sitting, I “hammered” the first through fourth thoracic vertebrae: first into right-to-left shear then left-to-right shear: both with some cervical flexion and ipsilateral rotation.
We then returned to supine on the table to re-assess cervical, I was hoping for at least a modest reduction in the painful myofascial tone on the right side cervical spine.
It was far less painful. In fact, it was nearly pain-free.
But more profound (if not bizarre): both uncovertebral and facet motion was completely restored, bilaterally.
In other words, we achieved 45 degrees of pain-free sideband and over 60 degrees of rotation, also pain-free: not from the preceding cervical treatment (that included joint glides), but from the thoracic (hammer) manipulation!
I might be easily amused, but I’m not easily surprised. A lot of odd things happen on my treatment table, on the regular.
But this was almost shocking. What felt like chronic, rigid, pre-arthritic joint mobility loss evaporated with a few taps of the hammer.
So what happened, exactly?
• did the thoracic shear loss somehow translate a similar effect into the cervical?
• did the thoracic vertebral stiffness create (and perpetuate) the high myofascial tone in the neck
• the ganglion of sympathetic nerves lives on the (front of the) upper thoracic spine. Did the vertebral stiffness of this upper column somehow cause a neuro-fascial tension that held both the myofascial and vertebral tissue “hostage”?
and thus treating the thoracic somehow “freed” this captive cervical spine?
However the mechanism, that outcome was clear.
He left moving and feeling better, and — given my uncertainty of the exact mechanism and whether or not the improvement would hold — we made plans to check in again next week.
Take-Aways. Treat the System (and the Foundations)! In my orthopedic manual training a couple things were heavily emphasized
• the impact of dysfunctional transitional junctions, particularly in the spine, and their widespread effects: craniocervical, cervico-thoracic, thoracolumbar, lumbopelvic.
• the relative sensitivity of the cervical and lumbar lordotic curves, from a stiff (and often too rigid and flexed) thoracic spine.
Thus evaluating and treating the upper thoracic for cervical cases is standard procedure for me. But seldom do I treat it so aggressively — particularly in a relatively acute strain event.
But seldom — if ever — have I experienced such a profound change in tissue tone and multi-segmental motion from a regional treatment, before.
For me, this was another “side door” attempt: an alternative mechanism to gain “access” to a very stiff, highly sensitive cervical spine. And boy, did I hit the jackpot!
So keep treating the system. And keep looking for those magical side doors that unlock crucial pain-free and functional motion!
Issue 128 is complete!
Help people move, function and feel better: please share this publication!
Thanks for reading, and have a great weekend,
Issue 106: Vitamins vs Coffee. Contrasting exercise intervention types between slow-acting (“vitamin”) and fast-acting (“coffee”). Vitamin-style exercises (cardio, stretching, or strength training) require weeks to years for gradual benefits, much like daily vitamins that offer delayed, hoped-for improvements. In contrast, coffee-style exercises provide fast-acting, layered effects—immediate gains in mobility, strength, and motor control, sustained improvements within days to weeks, and cumulative long-term benefits—making them more effective and motivating for short- to medium-term rehabilitation, especially for those people already “taking a lot of vitamins” (general physical activity and fitness).
Issue 32: Tight Hamstrings? It’s Your Quads! Due to the fascial nature of the thigh and the large size of the quadriceps, it is possible (if not commonplace) that excessive fascial tension (and tissue density) in the lateral quad may compress — or even adhere to — the hamstrings, laterally (and the same with the adductors, medially).




